Although the true origin of the Latin phase “Primum non nocere” (First, do no harm) is a little murky, the principle can be traced to at least Hippocrates (or one of his students) written in Ionic Greek 2,500 years ago, and as recently as likely ALL first year training in contemporary medical schools. How might this principle play out in pancreatic cancer, arguably the most aggressive of malignant tumors?
A recent study by Michael Wallace, MD, MPH and colleagues from the Mayo Clinic examined the records and outcomes of more than two thousand patients who received surgery for “locoregional” (roughly: locally advanced) pancreatic cancer via SEER [Surveillance, Epidemiology, and End Results] cancer patient data to evaluate the possible advantage or disadvantage of obtaining a fine needle biopsy through the bowel wall to reach the tissue of a suspected pancreatic tumor to aid in the diagnosis of pancreatic cancer. For the purposes of this study, pancreatic cancer was defined as an adenocarcinoma, mucinous cystadenocarcinoma, intraductal papillary mucinous carcinoma of the pancreas, malignant endocarcinoma, or malignant carcinoid tumor.
Wallace and colleagues published the results of their work in the July issue of the well-named journal Gut (one of the British Medical Journal publications).
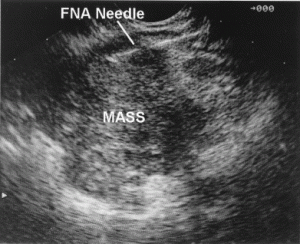
The use of a fine needle aspiration per esophageal ultrasound (EUS-FNA) is fast, relatively easy to perform, relatively benign as procedures tend to go, and could spare many patients much more intrusive procedures on the way to diagnosis. However, there has been a sense in the oncology community that the use of a needle to obtain a possible malignant tissue specimen and pulling that tissue via needle through body walls, space and other tissue may well “seed” the needle track with pancreatic cancer and even, for example, the peritoneum with in effect ready-made malignant metastases. Thus, this would violate perhaps the cardinal rule in medicine – do no harm. Several cases of such pancreatic cancer needle track seeding are present in the medical literature, but each of these is of cancer either from the body or the tail of the pancreas. There have been no reported cases related to FNA of pancreatic cancer from the head of the pancreas. So, the results of this current study are timely and perhaps more interesting and resonant than may first appear.
2,034 patients were identified by the researchers from the SEER database who met the study criteria of logoregional pancreatic cancer. All of the patients were aged 66 years or older, as this was a U.S. Medicare cohort. 76% of the patients (1,536) were in the (non)EUS-FNA arm and 24% (498) were in the EUS-FNA arm. 90% of the patients had adenocarcinoma of the pancreas. During the average (mean) review period of twenty-one months, 76% (1167) of the patients in the (non)EUS-FNA arm, and 57% (285) in the EUS-FNA arm died.
At analysis, the researchers found that the use of EUS-FNA was somewhat mildly associated with overall survival (but not cancer-specific survival). More importantly, the study data appears to show that the EUS-FNA procedure can be safely utilized as a part of the diagnostic work-up and evaluation for pancreatic cancer.
This gives impetus toward the use of EUS-FNA as a possible less intrusive aid for the diagnosis or exclusion of pancreatic cancer. The study may not be definitive, but gives comfort for a current indication. In time, more direct studies will undoubtedly offer better understandings as to more indications and contraindications related to the utilization of this procedure.
Dale O’Brien, MD